





اخبار و اطلاعیه های بیمارستان فوق تخصصی چشم پزشکی بینا

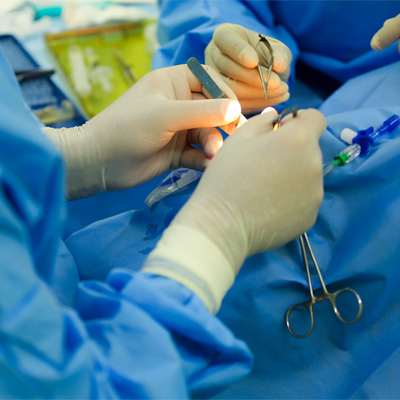
گرامیداشت روز علوم آزمایشگاهی

روز شمار هفته سلامت 1403

کنفرانس ماهیانه بیمارستان بینا

حساسیت های چشمی آلرژیک
گرامیداشت روز علوم آزمایشگاهی
30 فروردین ماه همزمان با گرامیداشت سالروز تولد دانشمند فرزانه ایرانی، حکیم جرجانی بنیان گذار و پدر علوم آزمایشگاهی، به عنوان روز آزمایشگاه و علوم آزمایشگاهی نامگذاری شده است. این روز بهانهای است برای قدردانی از تلاش های جامعه بزرگ علوم آزمایشگاهی کشور که همواره در راه...
روز شمار هفته سلامت 1403
هفته اول اردیبهشت ماه، هفته سلامت، گرامی باد وزارت بهداشت درمان و آموزش پزشکی (سلامت خانواده و مردمی سازی سلامت) را شعار این هفته تعیین کرده است. از جمله اهداف شعار هفته سلامت امسال می توان به موضوعات ذیل اشاره کرد: > حمایت طلبی و پررنگ نمودن ضرورت...
کنفرانس ماهیانه بیمارستان بینا
سخنران: دکتر آرش امیدتبریزی، جراح فوق تخصص شبکیه تاریخ و محل برگزاری: 30 فروردین ماه 1403 سالن همایشهای بیمارستان بینا موضوع: مبانی تفسیر OCTA جلسات علمی بینا با هدف تبادل اطلاعات روز دنیا با حضور جمعی از چشم پزشکان مجرب مشهد به صورت ماهیانه و حضوری از ساعت...
حساسیت های چشمی آلرژیک
بسیاری از حساسیت های چشمی یا آلرژی های چشمی که برخی از انواع آن ها به صورت التهاب ملتحمه بروز میکنند، واگیردار است با آغاز فصل بهار، طبیعت به زیبایی خود بازمیگردد. اما این فصل میتواند برای بسیاری از ما به چالش نیز تبدیل گردد. با تغییرات طبیعت که نه تنها موجب...
چرا بیمارستان فوق تخصصی چشم پزشکی بینا ؟
- کادر مجرب و آموزش دیده
- حذف عینک
- اورژانس تخصصی چشم
- تجهیزات پیشرفته و تخصصی
- پزشکان مجرب
- سامانه هوشمند HIS
- نوبت دهی هوشمند
کادر مجرب و آموزش دیده
بسیاری از متخصصین ما در عرصههای بینالمللی فعالیت میکنند و بیمارستان فوق تخصصی چشم پزشکی بینا با وجود امکانات درمانی مدرن و استاندارد باعث شده که بتوان از حداکثر توان این متخصصین بهره برد. هدف بیمارستان چشم بینا ارائه خدمات چشم پزشکی به روز با رعایت کرامت انسانی مراجعین محترم میباشد. از این رو پرسنل آموزش دیده تکریم و خدمات در بدو ورود به راهنمایی مراجعین محترم میپردازند. این بیمارستان با بهرهمندی از پرسنل مجرب و آموزش دیده و چشم پزشکان برجسته ایران و همچنین استفاده از تجهیزات جدید و پیشرفته چشم پزشکی، در حال خدمت رسانی به مراجعین محترم مشهد و سایر نقاط ایران و گردشگران سلامت میباشد.

 فارسی
فارسی العربية
العربية